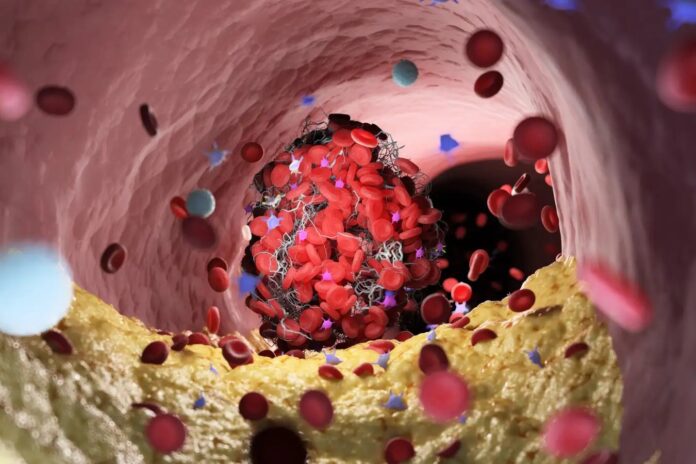
A breakthrough in cellular engineering may soon transform how surgeons manage life-threatening hemorrhages. Researchers have developed a method to modify red blood cells, turning them into a highly efficient, rapid-acting clotting agent that can stop severe bleeding almost instantly.
The Critical Problem: The Fatal Gap in Clotting
Every year, approximately 2 million people die worldwide due to blood loss. In medical emergencies, time is the most decisive factor; the longer a patient bleeds, the higher the risk of death.
While the human body is naturally designed to clot, severe trauma can overwhelm this system. Current medical interventions often face significant hurdles:
– Blood transfusions are expensive, logistically difficult to deliver quickly, and not always available in emergencies.
– Synthetic bandages can sometimes trigger adverse immune reactions or hinder the natural healing process.
The Innovation: Making Cells “Stickier”
In a study led by Jianyu Li at McGill University, researchers looked at the fundamental components of a blood clot. Normally, red blood cells, platelets, and a protein called fibrin work together to create a “plug” at the site of an injury. However, red blood cells are inherently fragile, which can limit the strength and duration of a natural clot.
The research team found a way to reinforce these cells by treating them with specialized chemical “handles.”
1. Attachment: One side of the chemical attaches to the surface of the red blood cells.
2. Linking: The other side is designed to bond with long-chain molecules that act as a bridge, linking the cells together into a much tougher structure.
Dramatic Results in Laboratory Trials
The effectiveness of this “engineered” blood was tested on rats with severe liver wounds, and the results were stark when compared to untreated subjects:
| Metric | Untreated Rats | Treated Rats |
|---|---|---|
| Clotting Time | ~265 seconds | < 5 seconds |
| Blood Loss | ~2,000 mg | ~24 mg |
Beyond speed, the durability of these engineered clots was a significant finding. While natural clots typically dissolve within a few days, these modified clots lasted between one and two months without causing safety concerns. This extended lifespan could provide a stable environment for wound-healing molecules to repair tissue more effectively.
Challenges and the Path to Clinical Use
While the results are promising, transitioning this technology from a lab setting to a hospital bedside involves several hurdles.
Implementation Scenarios
The researchers envision two primary ways this could be used:
– Planned Surgeries: A patient’s own blood could be collected, modified, and reinjected in under 30 minutes before an operation.
– Emergency Situations: Modified blood could be prepared in advance from blood banks and kept in refrigeration for at least a month.
The “Shelf Life” Obstacle
A key challenge remains the biological nature of the treatment. Unlike synthetic clotting agents, which can be stored for long periods, cellular materials are living components that may have a shorter shelf life. Experts note that for this to be a viable emergency tool, researchers must ensure the modified cells remain stable and effective over time.
“It is exciting work that shows a new design method for cell-based biomaterials for surgical and regenerative applications.” — Hyunwoo Yuk, founder of SanaHeal
Conclusion
By re-engineering the very cells that carry oxygen, scientists have created a way to turn blood into a high-speed surgical tool. If successfully transitioned to human use, this technology could bridge the critical gap between injury and stabilization, saving countless lives in the operating room.