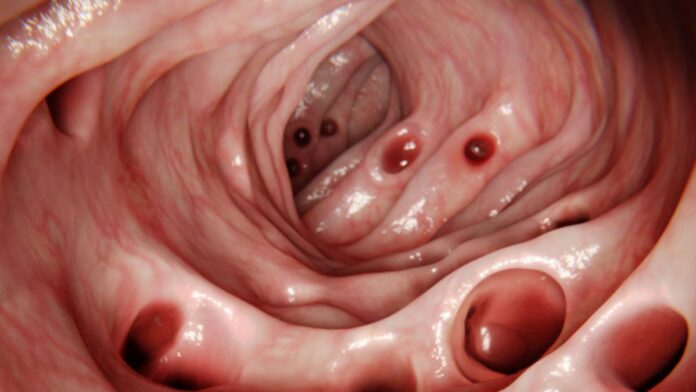
As we age, visible signs like wrinkles and gray hair are expected. However, internal changes are equally inevitable. By the age of 80, the majority of people develop diverticulosis —a condition characterized by small, bulging pouches in the lining of the digestive tract.
While the term sounds alarming, diverticulosis is typically harmless and often asymptomatic. Understanding the difference between these silent pouches and their inflamed counterparts is crucial for managing long-term gut health.
The Anatomy of Diverticula
Diverticula are sac-like protrusions that form in the muscular wall of the intestine. Think of them as weak spots where the inner lining pushes outward through the muscle layer.
- Diverticulosis: The mere presence of these pouches. Most people are unaware they have them until discovered incidentally during a colonoscopy for other reasons.
- Diverticulitis: The condition occurs when these pouches become inflamed or infected. This is the “disease” state that causes symptoms and requires medical attention.
To simplify the distinction, gastroenterologist Janyll Castineira from the University of Miami suggests a mnemonic: Diverticul‘O’osis refers to p‘O’ckets, while Diverticul‘I’itis refers to ‘I’nflammation.
Symptoms and Treatment
When diverticulitis develops, symptoms can fluctuate but often include:
* Abdominal pain (typically on the lower left side)
* Fever
* Nausea
* Changes in bowel habits, such as constipation or diarrhea
* Bloating
The Good News: The vast majority of cases are mild. According to clinical data, over 85% of patients recover fully with conservative treatment within a few days. This usually involves:
1. Bed rest.
2. A clear liquid diet to allow the gut to heal.
3. Over-the-counter pain management.
Antibiotics are prescribed selectively, and surgery is reserved for rare, severe complications such as abscesses or ruptures. Even in surgical cases, outcomes are generally excellent, with roughly 90% of patients remaining symptom-free after the removal of the affected intestine section.
Why Does This Happen? The Role of Diet and Pressure
The exact cause of diverticula formation remains a subject of ongoing research, but current evidence points to a combination of mechanical pressure and dietary habits.
In the Western world, diverticula most commonly form in the sigmoid colon (the lower part of the large intestine). This section operates under high pressure to move stool toward the rectum. When stool is hard or difficult to pass, the pressure increases, potentially forcing the lining to bulge outward.
“No one knows exactly what causes diverticula to form in the first place, but current treatments generally focus on helping the digestive tract move smoothly, without blockages.”
The Fiber Connection
Diet plays a pivotal role in both prevention and management. A high-fiber diet (25–30 grams per day) is the standard recommendation. While fiber cannot heal existing diverticula, it softens stool and reduces intestinal pressure, potentially preventing new pouches from forming.
- Global Disparity: Diverticulosis is prevalent in Western countries (US, UK, Australia) where diets are often low in fiber. Conversely, it is rare in Africa and Asia, where traditional diets are fiber-rich.
- Risk Reduction: The UK’s National Health Service (NHS) notes that individuals aged 50–70 with high fiber intake have a 40% lower risk of hospitalization for diverticular disease compared to those with low intake.
Emerging Research: The Gut Microbiome
Recent studies suggest that the mechanics of digestion may have broader health implications. A 2023 review highlighted distinct differences in the gut microbiomes of individuals with fast transit times (“speeders”) versus slow transit times (“slowpokes”). Since the microbiome is intrinsically linked to overall health, these variations could influence how diverticula form and behave, though this area remains controversial and requires further investigation.
Other established risk factors include:
* Obesity
* Physical inactivity
* Smoking
A Warning on Bleeding
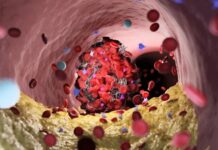
While diverticulosis is often silent, diverticular bleeding is a significant complication. It accounts for an estimated 30% to 65% of all lower gastrointestinal bleeding cases.
This bleeding is typically painless and may stop on its own, but it should never be ignored. Blood in the stool can also signal more severe conditions, such as colorectal cancer or inflammatory bowel disease. Medical guidance is essential if you notice blood in your stool, regardless of whether you suspect it is related to diverticula.
Conclusion
Diverticulosis is a common, natural part of aging for many, but it does not dictate a life of illness. By maintaining a high-fiber diet, staying active, and monitoring for symptoms like pain or bleeding, most individuals can manage this condition effectively. While the science continues to evolve regarding the precise causes and microbiome connections, the core advice remains simple: keep your digestive tract moving smoothly to protect your gut health.